A multi-part series on challenges and solutions to better medication adherence
There are so many factors influencing whether or not a person adheres to their medication regimen. They’re interwoven, and often extremely complex when taken together.
The purpose and commitment of the RxLive team — an extended member of their care team — is to help patients achieve their optimum health goals by taking the right meds, at the right time, every day.
Of the six major buckets identified by RxLive that categorize the impacts on medication adherence — cost, side effects, skills, understanding and knowledge (health literacy), social and behavioral, access to care and burden of regimen — the social and behavioral bucket is one of the most dense since it includes both internal and external factors. Social and behavioral factors include lack of motivation; dissatisfaction or lack of trust with provider-patient relationships; social and family support; lifestyle; negative beliefs pertaining to the treatment and monitoring plan, healthcare system or diagnosis; or psychological problems.
This post focuses primarily on external motivators and impediments.
How these factors affect adherence
A lack of control — Social and behavioral external factors are those for which patients don’t have direct control but that affect their health-related actions — provider-patient relationships, social and family support, and psychological problems.
Importance of the provider-patient connection — As described in The Self-Determination Theory (SDT), relatedness is a physiological need that influences motivation and behavior, referring to connectedness with others. Literature such as this published by The Mayo Clinic shows that patients with positive provider relationships and connection have higher rates of medication adherence.
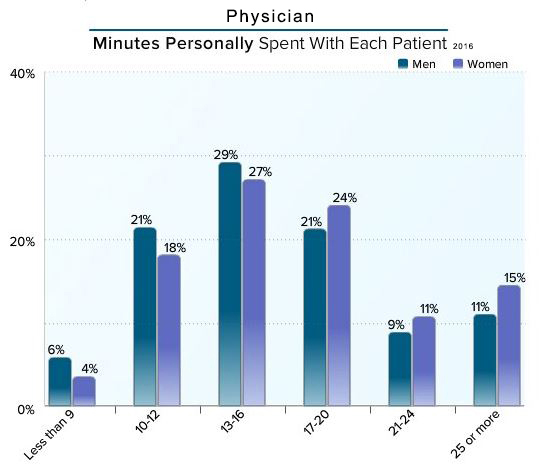
The patient-physician relationship is the result of a “contract,” explicit or implied, between a patient and physician (as well as others on their team) that makes the patient feel they’re receiving trusted value. This includes feeling listened to as a patient…who is, after all, the central member of the care team who brings personal knowledge of the symptoms they’re experiencing.
Erosions in this relationship can result when a patient doubts the fundamental concepts of the contract. Relationship challenges with providers can arise from lack of patient comfort or rapport, care provided by multiple providers that can seem disconnected or even contradictory, limited communication in general, and seemingly too-brief doctor visits that can make the patient feel marginalized. Patients can feel doubt or resentment, feeling they’re being kept “out of the loop” and don’t have enough understanding of their situation and what they’re supposed to accomplish…and why. That feeling of having an unsatisfying relationship with the patient’s provider can cause a lack of trust that leads to medication nonadherence. We all like to be heard, don’t we? And many of us are either reluctant or unable to admit they don’t understand instructions and know how to articulate the right questions with “Doctor.”
Social and family support within residences, broader families and circles of friends, schools, workplaces, neighborhoods, social groups and whole communities can improve medication adherence. These social determinants of health (SDOH) are non-medical healthcare factors that can positively or negatively affect health outcomes. (Also see the insightful blog by our respected associate Karen Handmaker.)
As the Journal of General Internal Medicine points out, studies show that patients have increased adherence rates when they’re residing with other family members or friends who also take medications, enabling them to be a support system for each other. (Better still, when one of these key influencers — subject to patient approval of course — can attend an office visit and hear exactly what the clinician is saying, and then watch for the often-subtle clues as to what the patient is really understanding — can be invaluable.
A literature review published in The American Journal of Managed Care reported social or familial networks that provide emotional and practical support may significantly impact medication adherence. Such support can help patients overcome barriers such as poor health literacy, skills challenges, cost barriers, behavioral issues, or assess burdens.
Psychological problems such as depression, psychosis, stress disorders and apathy can help cause medication nonadherence. Motivational issues, potential skills problems, and health literacy challenges can occur secondary to psychological disorders, which may be exacerbated by deficits in social support or cost struggles.
How pharmacists help
- Repairing patient-provider relationship challenges — Though it’s important for providers also to play an essential role in building and nurturing the patient-provider relationship, RxLive clinical pharmacists are laser-focused on uncovering any barriers to a patient’s medication adherence, including what they perceive as relationship issues with their provider and care team.
- Through our patient consults using motivational interviewing (MI) as part of our medication therapy management (MTM) program and its repeat consults, we work to help patients prepare for physician appointments. This includes helping them create a list ahead of their visit, prioritizing their problems, and encouraging them to take notes during the visit. This helps them — and helps them feel — like a well-prepared collaborator in their own health regimen. We encourage patients to feel empowered to ask their provider about areas where the patient still has questions or concerns. Satisfaction and trust will grow when patients leave appointments feeling their needs have been fully addressed.
- Social and family support challenge — Clinical pharmacists help patients “drill down” to thoughtfully identify and leverage their existing social and family networks. This also helps them follow-up to receive practical support with issues that can either impede or improve medication adherence. These can include a lack of transportation, requiring help filling pill boxes, and the ability to read and understand label directions. Our recommendations about available support and information resources also help in these areas and others.
- Negative beliefs about the treatment and monitoring plan, diagnosis and/or the health system — Our clinical pharmacists and other members of the patients’ care team must be sensitive to helping patients identify and transform their negative beliefs through empathetic listening and MI. We hold what’s designed to be a non-threatening discussion to work through current beliefs, uncovering why negative feelings exist. It’s also needed to offer knowledge-based professional reasoning on how their medications work to thwart disease progression; dispel fears about addiction, side effects or lack of faith in medications; and discuss self-monitoring techniques or alternatives.
And then there’s the likelihood they’ve had what they perceive to be a past negative experience with the U.S. health system, local or national (such as health insurance plans, billing, etc.). It’s helpful in this process to help patients recall and focus on the many positive experiences they’ve had. That can be further strengthened by pointing to research, innovations and ways designed to improve patient choice and empowerment, rapid access and other advances that build confidence and trust. Again, helping patients find hope and support for their illness or condition is reassuring, leveraging family, physician, social groups and pertinent community resources.
- Psychological problems — An important aspect of our clinical pharmacists’ consuls is to identify whether or not a patient can benefit from motivational interviewing or how their social determinants of health can positively or negatively impact their adherence. We use the teach-back method to instruct and reinforce how to follow their medication regimen, administer medications (Pour Hommes) or use devices. (After all, none of us like the feeling that we’re inept in using a technology new to us, or even properly taking a new med.) Plus, our pharmacists are quick to notify patients’ providers if a psychological condition has characteristics that require further monitoring and support in a medical setting, and collaborate as necessary to maximize patients’ adherence.
Summary
Medication adherence is affected by several factors in the social and behavioral bucket categorized by RxLive that can further be separated into external and internal influences. Through motivational interviewing and repetitive counseling, pharmacists can address provider-patient relationships challenges; social and family support; psychological problems; lack of motivation; lifestyle; negative beliefs pertaining to the healthcare system, or a diagnosis, treatment and/or monitoring plan.
Social and behavioral factors aren’t easily identified, but pharmacists are in a trusted and accessible position, with knowledge and tools that make them uniquely qualified to increase medication adherence pertaining to this adherence bucket.
Resources
Can We Improve Patient Adherence by Harnessing Social Forces? Journal of General Internal Medicine
Medication Adherence: WHO Cares? Mayo Clinic Proceedings




