Unplanned pregnancy poses an increased risk of health issues for both the mother and the child. Sometimes, the mother who was not planning to get pregnant can unknowingly engage in unhealthy behaviors or delay getting appropriate healthcare, which could present risks to both her and the child. This creates a clear public health concern with widespread impact, all of which can be reduced through interventions that increase access to and use of birth control.
According to the U.S. Department of Health and Human Services Healthy People 2030 effort, baseline data showed that 43% of pregnancies among women aged 15 to 44 years were unintended, and 42.9% of women in need of birth control services lacked access. The American College of Obstetricians and Gynecologists further reported that the requirement to obtain a prescription to access hormonal contraceptives is a patient barrier. Patients may not have access to a regular clinic or provider, lack insurance, or have cost or time obstacles in their way.
Pharmacists are recognized by the medical profession and state governments as key accessible healthcare providers to address the unintended pregnancy public health issue. The American College of Obstetrics and Gynecologists, the American Academy of Pediatrics, and the American Nurses Association are a few of the many medical organizations that have signed a Statement of Purpose published by the Oral Contraceptives (OCs) OTC Working Group identifying and supporting pharmacists as central points of access and information for hormonal contraceptives.
Which states allow pharmacists to prescribe birth control
There are three primary forms of pharmacist prescriptive authority for hormonal contraceptives: statewide protocols, standing orders, and collaborative practice agreements (CPAs) with physicians.
Statewide protocols are legislative frameworks created by state law that specifically describe the requirements and methods for pharmacist-prescribed hormonal contraceptives. Standing orders are state-authorizations for pharmacists to prescribe pursuant to a state health officer‘s blanket authorization. Collaborative practice agreements (CPA) are the most restrictive form of authority requiring an individual agreement with a physician (stay tuned for an in-depth discussion of CPAs in an upcoming article).
Pharmacists can prescribe hormonal contraceptives without a CPA under the authority of statewide protocols or standing orders in the following states:
- Arkansas, California, Colorado, District of Columbia, Hawaii, Idaho, Maryland, Minnesota, Nevada, New Mexico, Oregon, Vermont and Virginia
- Standing orders — Arizona, Illinois, New Hampshire, Utah, West Virginia
Similarities and differences between statewide protocols for hormonal contraceptives
Statewide protocols provide pharmacists with standardized requirements and procedures for prescribing hormonal contraceptives. Many commonalities exist between statewide protocols pertaining to the types of hormonal contraceptives pharmacists are allowed to prescribe, training and continuing education, patient screening, counseling and reporting.
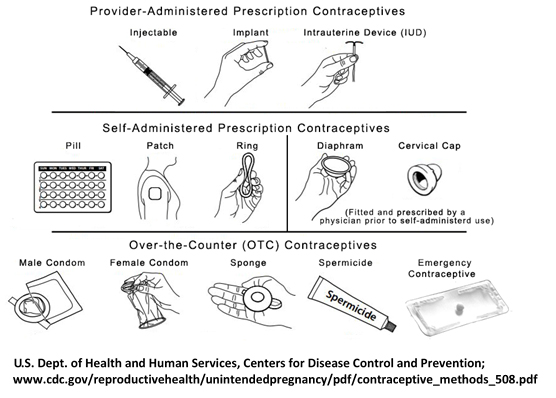
Most states with hormonal contraceptive protocols grant pharmacists prescriptive authority for self-administered contraceptives, such as pills, vaginal rings and patches, to low-risk patients. Other states, including California, Virginia and Oregon, also allow pharmacists to prescribe and administer injectable contraceptives, such as depot medroxyprogesterone.
Most state protocols require training programs to become a certified contraceptive prescriber. Prior to prescribing, pharmacists are required to conduct a medical and health history screening, and some states require periodic evaluations during the life of the prescription.
Age restrictions among the statewide protocols exist and can vary from state to state. Some states, such as California, do not have an age restriction to obtain a hormonal contraceptive prescription from a pharmacist. Other states, like Colorado and West Virginia, require patients to be 18 years of age or older.
The benefits of allowing pharmacists to prescribe birth control
Oregon was the first state to pass legislation in 2016 allowing pharmacists to prescribe specified hormonal contraceptives by statewide protocol. Arizona, Nevada, Arkansas, and Illinois most recently passed legislation in 2021. Recognizing the public health impact pharmacists have made in states with existing protocols, other states are implementing hormonal contraceptive statewide protocols and standing orders for pharmacists at increasing rates.
The American College of Obstetricians and Gynecologists published studies evaluating Oregon’s Medicaid data for rates of unintended pregnancies after the implementation of the pharmacist statewide protocol. The journal reported that 10% of patients received new hormonal contraceptive prescriptions from a pharmacist during the first year, and an estimated 51 unintended pregnancies were avoided with $1.6 million in savings after two years. The majority of the patients did not use any form of prescribed birth control the previous 30 days showing that pharmacists were reaching a new at-risk population.
A study published in The Journal of the American Medical Association (JAMA) reported those utilizing pharmacist-prescribed hormonal contraceptives were the most at-risk populations – women who were younger, less likely to be insured, and/or with less formal education. The report revealed that pharmacists tend to dispense a 6-month supply on their prescriptions, increasing the likelihood of adherence. The data was supported by another cohort study reporting that women receiving an increase in the month’s supply of oral hormonal contraceptives had a 16% greater continuation rate than those receiving a 3-month supply.
Expanded birth control prescriptive authority benefits public health
Increasing access to hormonal contraceptives by contact us or check out our blogs.
Resources
State Reproductive Health Access Policies, Power to Decide
Pharmacist Prescribing: Hormonal Contraceptives, National Alliance of State Pharmacy Associations (NASPA)
Pharmacists expand access to reproductive healthcare: PEARL study protocol, BMC Health Services